Pes Planus?
Overview

Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
It?s possible to have fallen arches and experience no symptoms whatsoever. But many people do notice some problems with this condition. Their feet, back and legs ache. Standing on their toes is difficult, if not impossible, and they note swelling around the arch and heel.
Diagnosis
Many medical professionals can diagnose a flat foot by examining the patient standing or just looking at them. On going up onto tip toe the deformity will correct when this is a flexible flat foot in a child with lax joints. Such correction is not seen in the adult with a rigid flat foot. An easy and traditional home diagnosis is the "wet footprint" test, performed by wetting the feet in water and then standing on a smooth, level surface such as smooth concrete or thin cardboard or heavy paper. Usually, the more the sole of the foot that makes contact (leaves a footprint), the flatter the foot. In more extreme cases, known as a kinked flatfoot, the entire inner edge of the footprint may actually bulge outward, where in a normal to high arch this part of the sole of the foot does not make contact with the ground at all.
how to fix fallen arches
Non Surgical Treatment
During walking and running, there is a small natural inward drop (slight pronation) that is part of the spring and propulsion. Allowing exaggerated sagging is like rounding your shoulders too much. Legs and feet have posture that you can control yourself. Use your own muscles and get free built-in exercise and arch support all day, and stop painful poor positioning. Some people with existing abnormality or growths in the ball of the foot will roll inward (or outward) to get the pressure off the deformed area because standing straight hurts. See your doctor first. Remember, don't force. If it hurts, it's wrong. All you are doing is learning how to stand neutral, not tilted so much that you compress the joints. The concept is to hold your feet in the same healthful position that shoe supports would. It is like an ice skater holds their skates straight at the ankle, not angled.
Surgical Treatment

Generally one of the following procedures is used to surgically repair a flat foot or fallen arch. Arthrodesis. One or more of your bones in the foot or ankle are fused together. Osteotomy. Correcting alignment by cutting and reshaping a bone. Excision. Removing a bone or a bone spur. Synovectomy. Cleaning the sheath that covers the tendon. Tendon transfer. Using a piece of one tendon to lengthen or replace another. Arthroereisis. placing a small device in the subtalar joint to limit motion. For most people, treatment is successful, regardless of the cause, although the cause does does play a major role in determining your prognosis. Some causes do not need treatment, while others require a surgical fix.
Prevention
oll away pain. If you're feeling pain in the arch area, you can get some relief by massaging the bottom of your foot. A regular massage while you're watching TV can do wonders" Stretch out. Doing the same type of stretching exercises that runners do in their warm-up can help reduce arch pain caused by a tight heel cord. One of the best exercises is to stand about three feet from a wall and place your hands on the wall. Leaning toward the wall, bring one foot forward and bend the knee so that the calf muscles of the other leg stretch. Then switch legs. Stretching is particularly important for women who spend all week in heels and then wear exercise shoes or sneakers on weekends. Get measured each time you buy new shoes. Don't assume that since you always wore a particular size, you always will. Too many people try to squeeze into their 'regular' shoe size and wind up with serious foot problems or sores on their feet. When your arch is falling, your feet may get longer or wider and you may or may not feel pain, so getting your foot measured each time you buy shoes is a good indicator of your arch's degeneration. Examine your shoes. If the heel is worn down, replace it. But if the back portion of the shoe is distorted or bent to one side, get yourself into a new pair of supportive shoes like those made specifically for walking. That's because flat feet can affect your walking stride, and failing to replace worn shoes may lead to knee or hip pain.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.

Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
It?s possible to have fallen arches and experience no symptoms whatsoever. But many people do notice some problems with this condition. Their feet, back and legs ache. Standing on their toes is difficult, if not impossible, and they note swelling around the arch and heel.
Diagnosis
Many medical professionals can diagnose a flat foot by examining the patient standing or just looking at them. On going up onto tip toe the deformity will correct when this is a flexible flat foot in a child with lax joints. Such correction is not seen in the adult with a rigid flat foot. An easy and traditional home diagnosis is the "wet footprint" test, performed by wetting the feet in water and then standing on a smooth, level surface such as smooth concrete or thin cardboard or heavy paper. Usually, the more the sole of the foot that makes contact (leaves a footprint), the flatter the foot. In more extreme cases, known as a kinked flatfoot, the entire inner edge of the footprint may actually bulge outward, where in a normal to high arch this part of the sole of the foot does not make contact with the ground at all.
how to fix fallen arches
Non Surgical Treatment
During walking and running, there is a small natural inward drop (slight pronation) that is part of the spring and propulsion. Allowing exaggerated sagging is like rounding your shoulders too much. Legs and feet have posture that you can control yourself. Use your own muscles and get free built-in exercise and arch support all day, and stop painful poor positioning. Some people with existing abnormality or growths in the ball of the foot will roll inward (or outward) to get the pressure off the deformed area because standing straight hurts. See your doctor first. Remember, don't force. If it hurts, it's wrong. All you are doing is learning how to stand neutral, not tilted so much that you compress the joints. The concept is to hold your feet in the same healthful position that shoe supports would. It is like an ice skater holds their skates straight at the ankle, not angled.
Surgical Treatment

Generally one of the following procedures is used to surgically repair a flat foot or fallen arch. Arthrodesis. One or more of your bones in the foot or ankle are fused together. Osteotomy. Correcting alignment by cutting and reshaping a bone. Excision. Removing a bone or a bone spur. Synovectomy. Cleaning the sheath that covers the tendon. Tendon transfer. Using a piece of one tendon to lengthen or replace another. Arthroereisis. placing a small device in the subtalar joint to limit motion. For most people, treatment is successful, regardless of the cause, although the cause does does play a major role in determining your prognosis. Some causes do not need treatment, while others require a surgical fix.
Prevention
oll away pain. If you're feeling pain in the arch area, you can get some relief by massaging the bottom of your foot. A regular massage while you're watching TV can do wonders" Stretch out. Doing the same type of stretching exercises that runners do in their warm-up can help reduce arch pain caused by a tight heel cord. One of the best exercises is to stand about three feet from a wall and place your hands on the wall. Leaning toward the wall, bring one foot forward and bend the knee so that the calf muscles of the other leg stretch. Then switch legs. Stretching is particularly important for women who spend all week in heels and then wear exercise shoes or sneakers on weekends. Get measured each time you buy new shoes. Don't assume that since you always wore a particular size, you always will. Too many people try to squeeze into their 'regular' shoe size and wind up with serious foot problems or sores on their feet. When your arch is falling, your feet may get longer or wider and you may or may not feel pain, so getting your foot measured each time you buy shoes is a good indicator of your arch's degeneration. Examine your shoes. If the heel is worn down, replace it. But if the back portion of the shoe is distorted or bent to one side, get yourself into a new pair of supportive shoes like those made specifically for walking. That's because flat feet can affect your walking stride, and failing to replace worn shoes may lead to knee or hip pain.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
All You Will Need To Know About Heel Aches
Overview

Heel pain is one of the most common conditions to affect the foot. It is usually felt as an intense pain when the affected heel is used. The pain is usually worse when you get out of bed in the morning or after a long period of activity. In most cases, only one heel is affected. After walking, the pain usually improves. However, it is common for it to be painful when you first take a step after a period of rest. The pain often worsens by the end of the day. Most cases of heel pain are caused by damage and thickening of the plantar fascia. Sometimes, the surrounding tissue and the heel bone also become inflamed (swollen).
Causes
There are many reasons why people experience heel pain. Based on what we see in our office, heel pain affects, probably more than one in every four people. A lot of this is caused from conditions within the foot. These conditions could be related to hyper pronation, which is where you get a collapse of the foot or even a high arch of the foot called cavus foot. The underlying cause is something internal, within the bone structure. These problems are usually something you will have all your life. Hyper pronation is a hereditary issue where you can get an under development of a particular bone, usually in the ankle, and it causes a dislocation or a misalignment of the ankle on the heel. It throws off, not only the foot with the bones, joints and ligaments of the foot, but also the bones in the ankle. It affects the internal rotation of the knee, hip, back and causes issues within those areas as well. Hyper pronation is a pretty common, but very under diagnosed condition.
Symptoms
Symptoms include a dull ache which is felt most of the time with episodes of a sharp pain in the centre of the heel or on the inside margin of the heel. Often the pain is worse on first rising in the morning and after rest and is aggravated by prolonged weight bearing & thin soled shoes.
Diagnosis
In most cases, your GP or a podiatrist (a specialist in foot problems and foot care) should be able to diagnose the cause of your heel pain by asking about your symptoms and medical history, examining your heel and foot.
Non Surgical Treatment
Using our state-of-the-art equipment, Dr. Weinert is able to provide a full work up for the heel, including gait analysis. Digital imagining gives him and the patient a full view of the foot and injury to help formulate the best treatment plan possible. There are numerous treatment options available to help with heel pain and plantar fasciitis. Anti-inflammatory medications. Digital custom orthotics. Physical therapy. Diagnostic and ultrasonic guided injection therapy. No one should ever resign to living with foot pain.
Surgical Treatment
Only a relatively few cases of heel pain require surgery. If required, surgery is usually for the removal of a spur, but also may involve release of the plantar fascia, removal of a bursa, or a removal of a neuroma or other soft-tissue growth.
heel cushions for plantar fasciitis
Prevention

Preventing heel pain is crucial to avoid pain that can easily interrupt a busy or active lifestyle. Athletes can prevent damage by stretching the foot and calf both before and after an exercise routine. The plantar fascia ligament can be stretched by using a tennis ball or water bottle and rolling it across the bottom of the foot. With regular stretching, the stretching and flexibility of tissue through the foot can be significantly improved, helping to prevent damage and injury. Athletes should also ease into new or more difficult routines, allowing the plantar fascia and other tissue to become accustomed to the added stress and difficulty. Running up hills is also common among athletes in their routines. However, this activity should be reduced since it places an increased amount of stress on the plantar fascia and increases the risk of plantar fasciitis. Maintaining a healthy weight is also an essential heel pain prevention technique. Obesity brings additional weight and stress on the heel of the foot, causing damage and pain in the heel as well as in other areas of the foot.

Heel pain is one of the most common conditions to affect the foot. It is usually felt as an intense pain when the affected heel is used. The pain is usually worse when you get out of bed in the morning or after a long period of activity. In most cases, only one heel is affected. After walking, the pain usually improves. However, it is common for it to be painful when you first take a step after a period of rest. The pain often worsens by the end of the day. Most cases of heel pain are caused by damage and thickening of the plantar fascia. Sometimes, the surrounding tissue and the heel bone also become inflamed (swollen).
Causes
There are many reasons why people experience heel pain. Based on what we see in our office, heel pain affects, probably more than one in every four people. A lot of this is caused from conditions within the foot. These conditions could be related to hyper pronation, which is where you get a collapse of the foot or even a high arch of the foot called cavus foot. The underlying cause is something internal, within the bone structure. These problems are usually something you will have all your life. Hyper pronation is a hereditary issue where you can get an under development of a particular bone, usually in the ankle, and it causes a dislocation or a misalignment of the ankle on the heel. It throws off, not only the foot with the bones, joints and ligaments of the foot, but also the bones in the ankle. It affects the internal rotation of the knee, hip, back and causes issues within those areas as well. Hyper pronation is a pretty common, but very under diagnosed condition.
Symptoms
Symptoms include a dull ache which is felt most of the time with episodes of a sharp pain in the centre of the heel or on the inside margin of the heel. Often the pain is worse on first rising in the morning and after rest and is aggravated by prolonged weight bearing & thin soled shoes.
Diagnosis
In most cases, your GP or a podiatrist (a specialist in foot problems and foot care) should be able to diagnose the cause of your heel pain by asking about your symptoms and medical history, examining your heel and foot.
Non Surgical Treatment
Using our state-of-the-art equipment, Dr. Weinert is able to provide a full work up for the heel, including gait analysis. Digital imagining gives him and the patient a full view of the foot and injury to help formulate the best treatment plan possible. There are numerous treatment options available to help with heel pain and plantar fasciitis. Anti-inflammatory medications. Digital custom orthotics. Physical therapy. Diagnostic and ultrasonic guided injection therapy. No one should ever resign to living with foot pain.
Surgical Treatment
Only a relatively few cases of heel pain require surgery. If required, surgery is usually for the removal of a spur, but also may involve release of the plantar fascia, removal of a bursa, or a removal of a neuroma or other soft-tissue growth.
heel cushions for plantar fasciitis
Prevention

Preventing heel pain is crucial to avoid pain that can easily interrupt a busy or active lifestyle. Athletes can prevent damage by stretching the foot and calf both before and after an exercise routine. The plantar fascia ligament can be stretched by using a tennis ball or water bottle and rolling it across the bottom of the foot. With regular stretching, the stretching and flexibility of tissue through the foot can be significantly improved, helping to prevent damage and injury. Athletes should also ease into new or more difficult routines, allowing the plantar fascia and other tissue to become accustomed to the added stress and difficulty. Running up hills is also common among athletes in their routines. However, this activity should be reduced since it places an increased amount of stress on the plantar fascia and increases the risk of plantar fasciitis. Maintaining a healthy weight is also an essential heel pain prevention technique. Obesity brings additional weight and stress on the heel of the foot, causing damage and pain in the heel as well as in other areas of the foot.
True Leg Length Discrepancy Tests
Overview
Large leg length inequalities can be treated by staged lengthenings or by simultaneous ipsilateral femoral and tibial lengthenings. Additionally, lengthenings can be combined with appropriately timed epiphysiodesis in an effort to produce leg length equality. Staged lengthenings are often used for congenital deficiencies such as fibular hemimelia, in which 15 cm or more may be needed to produce leg length equality. We typically plan for the final lengthening to be completed by age 13 or 14 years, and allow at least 3 years between lengthenings. Lengthening of both the tibia and femur simultaneously requires aggressive therapy and treatment of soft tissue contractures. Curran et al[57] reported the need for surgical release of soft tissue contractures in 3 of 8 patients treated with simultaneous ipsilateral femoral and tibial lengthenings. Lengthening over an IM nail can be done in an effort to decrease the amount of time the fixator needs to be worn and to prevent angular malalignment. This technique requires that the patient be skeletally mature and it carries a higher risk of osteomyelitis (up to 15%). Additionally, if premature consolidation occurs, a repeat corticotomy is more difficult.
Causes
An anatomical short leg is due to several orthopedic or medical condition mechanisms. Often, one leg simply stops growing before the other one does and is called ?congenital?. We often see mother-daughters or father-sons who exhibit virtually the same degree of shortness on the same side. Often it is not known why this occurs, but it seems to account for approximately 25% of the population demonstrating a true LLD. Other causes of a true LLD include trauma or broken bones, surgical repair, joint replacement, radiation exposure, tumors or Legg-Calves-Perthes disease.
Symptoms
In addition to the distinctive walk of a person with leg length discrepancy, over time, other deformities may be noted, which help compensate for the condition. Toe walking on the short side to decrease the swaying during gait. The foot will supinate (high arch) on the shorter side. The foot will pronate (flattening of the arch) on the longer side. Excessive pronation leads to hypermobility and instability, resulting in metatarsus primus varus and associated unilateral juvenile hallux valgus (bunion) deformity.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
For minor limb length discrepancy in patients with no deformity, treatment may not be necessary. Because the risks may outweigh the benefits, surgical treatment to equalize leg lengths is usually not recommended if the difference is less than 1 inch. For these small differences, the physician may recommend a shoe lift. A lift fitted to the shoe can often improve walking and running, as well as relieve any back pain that may be caused by the limb length discrepancy. Shoe lifts are inexpensive and can be removed if they are not effective.

how to increase height after 25
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
Large leg length inequalities can be treated by staged lengthenings or by simultaneous ipsilateral femoral and tibial lengthenings. Additionally, lengthenings can be combined with appropriately timed epiphysiodesis in an effort to produce leg length equality. Staged lengthenings are often used for congenital deficiencies such as fibular hemimelia, in which 15 cm or more may be needed to produce leg length equality. We typically plan for the final lengthening to be completed by age 13 or 14 years, and allow at least 3 years between lengthenings. Lengthening of both the tibia and femur simultaneously requires aggressive therapy and treatment of soft tissue contractures. Curran et al[57] reported the need for surgical release of soft tissue contractures in 3 of 8 patients treated with simultaneous ipsilateral femoral and tibial lengthenings. Lengthening over an IM nail can be done in an effort to decrease the amount of time the fixator needs to be worn and to prevent angular malalignment. This technique requires that the patient be skeletally mature and it carries a higher risk of osteomyelitis (up to 15%). Additionally, if premature consolidation occurs, a repeat corticotomy is more difficult.

Causes
An anatomical short leg is due to several orthopedic or medical condition mechanisms. Often, one leg simply stops growing before the other one does and is called ?congenital?. We often see mother-daughters or father-sons who exhibit virtually the same degree of shortness on the same side. Often it is not known why this occurs, but it seems to account for approximately 25% of the population demonstrating a true LLD. Other causes of a true LLD include trauma or broken bones, surgical repair, joint replacement, radiation exposure, tumors or Legg-Calves-Perthes disease.
Symptoms
In addition to the distinctive walk of a person with leg length discrepancy, over time, other deformities may be noted, which help compensate for the condition. Toe walking on the short side to decrease the swaying during gait. The foot will supinate (high arch) on the shorter side. The foot will pronate (flattening of the arch) on the longer side. Excessive pronation leads to hypermobility and instability, resulting in metatarsus primus varus and associated unilateral juvenile hallux valgus (bunion) deformity.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
For minor limb length discrepancy in patients with no deformity, treatment may not be necessary. Because the risks may outweigh the benefits, surgical treatment to equalize leg lengths is usually not recommended if the difference is less than 1 inch. For these small differences, the physician may recommend a shoe lift. A lift fitted to the shoe can often improve walking and running, as well as relieve any back pain that may be caused by the limb length discrepancy. Shoe lifts are inexpensive and can be removed if they are not effective.

how to increase height after 25
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
What Is Mortons Neuroma
Overview
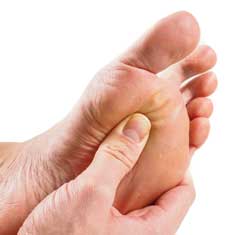 A Morton's neuroma is a benign (noncancerous) swelling along a nerve in the foot that carries sensations from the toes. The reason the nerve starts to swell is unknown. But once swelling begins, the nearby bones and ligaments put pressure on the nerve, causing more irritation and inflammation. This produces burning pain, numbness, tingling and other abnormal sensations in the toes. A Morton's neuroma also is called an interdigital neuroma, intermetatarsal neuroma or a forefoot neuroma.
A Morton's neuroma is a benign (noncancerous) swelling along a nerve in the foot that carries sensations from the toes. The reason the nerve starts to swell is unknown. But once swelling begins, the nearby bones and ligaments put pressure on the nerve, causing more irritation and inflammation. This produces burning pain, numbness, tingling and other abnormal sensations in the toes. A Morton's neuroma also is called an interdigital neuroma, intermetatarsal neuroma or a forefoot neuroma.
Causes
Poorly fitted footwear can be a cause. Shoes that have a tight and narrow toe box can cause the never to become entrapped causing the pain. High heeled shoes abnormally place the metatarsals under extreme pressure which can cause Morton?s Neuroma. In cases of abnormal pronation, there can be significant motion between the 3rd and 4th metatarsals which can cause an irritation to the nerve that runs between them. This inflammation causes the pain.
Symptoms
Patients will feel pain that worsens with walking, particularly when walking in shoes with thin soles or high heels. Also, anything that squeezes the metatarsal heads together may aggravate symptoms, such as narrow shoes. A patient may feel the need to remove the shoe and rub the foot to soothe the pain.
Diagnosis
You should visit a doctor or podiatrist (foot doctor) if you have pain or tingling that does not stop. Your health care provider will examine your feet and will apply pressure on the spaces between the bones of the toes to determine the location of the foot pain. The doctor may order X-rays to rule out other conditions associated with foot pain, such as a stress fracture or arthritis. X-rays alone will not show whether or not a neuroma is present, so an ultrasound scan or magnetic resonance imaging (MRI) test may be done to confirm the diagnosis. A diagnostic procedure called an electromyography is sometimes used to rule out nerve conditions that may cause symptoms like those of associated with Morton?s neuroma.
Non Surgical Treatment
In developing a treatment plan, your foot and ankle surgeon will first determine how long you?ve had the neuroma and evaluate its stage of development. Treatment approaches vary according to the severity of the problem. For mild to moderate neuromas, treatment options may include Padding techniques provide support for the metatarsal arch, thereby lessening the pressure on the nerve and decreasing the compression when walking. Placing an icepack on the affected area helps reduce swelling. Custom orthotic devices provided by your foot and ankle surgeon provide the support needed to reduce pressure and compression on the nerve. Activities that put repetitive pressure on the neuroma should be avoided until the condition improves. Wear shoes with a wide toe box and avoid narrow-toed shoes or shoes with high heels. Oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce pain and inflammation. Treatment may include injections of cortisone, local anesthetics or other agents.
Surgical Treatment
Surgery for mortons neuroma consists of either a decompression, where more space is created for the nerve or a resection, where this part of the nerve is removed completely. This will result in some permanent minor numbness. Success rates for surgical procedures to treat mortons neuroma have a high success rate.
 A Morton's neuroma is a benign (noncancerous) swelling along a nerve in the foot that carries sensations from the toes. The reason the nerve starts to swell is unknown. But once swelling begins, the nearby bones and ligaments put pressure on the nerve, causing more irritation and inflammation. This produces burning pain, numbness, tingling and other abnormal sensations in the toes. A Morton's neuroma also is called an interdigital neuroma, intermetatarsal neuroma or a forefoot neuroma.
A Morton's neuroma is a benign (noncancerous) swelling along a nerve in the foot that carries sensations from the toes. The reason the nerve starts to swell is unknown. But once swelling begins, the nearby bones and ligaments put pressure on the nerve, causing more irritation and inflammation. This produces burning pain, numbness, tingling and other abnormal sensations in the toes. A Morton's neuroma also is called an interdigital neuroma, intermetatarsal neuroma or a forefoot neuroma.Causes
Poorly fitted footwear can be a cause. Shoes that have a tight and narrow toe box can cause the never to become entrapped causing the pain. High heeled shoes abnormally place the metatarsals under extreme pressure which can cause Morton?s Neuroma. In cases of abnormal pronation, there can be significant motion between the 3rd and 4th metatarsals which can cause an irritation to the nerve that runs between them. This inflammation causes the pain.
Symptoms
Patients will feel pain that worsens with walking, particularly when walking in shoes with thin soles or high heels. Also, anything that squeezes the metatarsal heads together may aggravate symptoms, such as narrow shoes. A patient may feel the need to remove the shoe and rub the foot to soothe the pain.
Diagnosis
You should visit a doctor or podiatrist (foot doctor) if you have pain or tingling that does not stop. Your health care provider will examine your feet and will apply pressure on the spaces between the bones of the toes to determine the location of the foot pain. The doctor may order X-rays to rule out other conditions associated with foot pain, such as a stress fracture or arthritis. X-rays alone will not show whether or not a neuroma is present, so an ultrasound scan or magnetic resonance imaging (MRI) test may be done to confirm the diagnosis. A diagnostic procedure called an electromyography is sometimes used to rule out nerve conditions that may cause symptoms like those of associated with Morton?s neuroma.
Non Surgical Treatment
In developing a treatment plan, your foot and ankle surgeon will first determine how long you?ve had the neuroma and evaluate its stage of development. Treatment approaches vary according to the severity of the problem. For mild to moderate neuromas, treatment options may include Padding techniques provide support for the metatarsal arch, thereby lessening the pressure on the nerve and decreasing the compression when walking. Placing an icepack on the affected area helps reduce swelling. Custom orthotic devices provided by your foot and ankle surgeon provide the support needed to reduce pressure and compression on the nerve. Activities that put repetitive pressure on the neuroma should be avoided until the condition improves. Wear shoes with a wide toe box and avoid narrow-toed shoes or shoes with high heels. Oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce pain and inflammation. Treatment may include injections of cortisone, local anesthetics or other agents.

Surgical Treatment
Surgery for mortons neuroma consists of either a decompression, where more space is created for the nerve or a resection, where this part of the nerve is removed completely. This will result in some permanent minor numbness. Success rates for surgical procedures to treat mortons neuroma have a high success rate.
Shoe Lifts The Podiatrists Solution For Leg Length Discrepancy
There are not one but two different types of leg length discrepancies, congenital and acquired. Congenital means you are born with it. One leg is anatomically shorter compared to the other. As a result of developmental phases of aging, the brain picks up on the step pattern and identifies some variation. The body usually adapts by dipping one shoulder to the "short" side. A difference of under a quarter inch isn't very abnormal, require Shoe Lifts to compensate and in most cases doesn't have a profound effect over a lifetime.

Leg length inequality goes typically undiscovered on a daily basis, yet this condition is simply corrected, and can eradicate a number of cases of back pain.
Treatment for leg length inequality typically involves Shoe Lifts. They are low cost, in most cases costing under twenty dollars, in comparison to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lumbar pain is easily the most prevalent ailment afflicting people today. Around 80 million men and women are afflicted by back pain at some point in their life. It's a problem that costs businesses millions year after year as a result of lost time and output. Fresh and improved treatment solutions are constantly sought after in the hope of minimizing the economic influence this issue causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In a lot of these cases Shoe Lifts might be of very helpful. The lifts are capable of alleviating any pain and discomfort in the feet. Shoe Lifts are recommended by many experienced orthopaedic physicians.
So that you can support the human body in a balanced manner, feet have got a critical role to play. Despite that, it can be the most neglected zone of the body. Some people have flat-feet meaning there may be unequal force placed on the feet. This causes other areas of the body like knees, ankles and backs to be impacted too. Shoe Lifts make sure that the right posture and balance are restored.

Leg length inequality goes typically undiscovered on a daily basis, yet this condition is simply corrected, and can eradicate a number of cases of back pain.
Treatment for leg length inequality typically involves Shoe Lifts. They are low cost, in most cases costing under twenty dollars, in comparison to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lumbar pain is easily the most prevalent ailment afflicting people today. Around 80 million men and women are afflicted by back pain at some point in their life. It's a problem that costs businesses millions year after year as a result of lost time and output. Fresh and improved treatment solutions are constantly sought after in the hope of minimizing the economic influence this issue causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In a lot of these cases Shoe Lifts might be of very helpful. The lifts are capable of alleviating any pain and discomfort in the feet. Shoe Lifts are recommended by many experienced orthopaedic physicians.
So that you can support the human body in a balanced manner, feet have got a critical role to play. Despite that, it can be the most neglected zone of the body. Some people have flat-feet meaning there may be unequal force placed on the feet. This causes other areas of the body like knees, ankles and backs to be impacted too. Shoe Lifts make sure that the right posture and balance are restored.
Simple Methods To Diagnose Posterior Calcaneal Spur

Overview
The heel spur (or calcaneal spur) is a nail-like growth of calcium around the ligaments and tendons of the foot where they attach to the heel bone. The spur grows from the bone and into the flesh of the foot. A heel spur results from an anatomical change of the calcaneus (heel bone). This involves the area of the heel and occasionally, another disability, such as arthritis. The heel bone forms one end of the two longitudinal arches of the foot. These arches are held together by ligaments and are activated by the muscles of the foot (some of which are attached beneath the arches and run from the front to the back of the foot). These muscles and ligaments, like the other supporting tissues of the body, are attached in two places. Many are attached at the heel bone. The body reacts to the stress at the heel bone by calcifying the soft tissue attachments and creating a spur.
Causes
Diseases such as arthritis may lead to chronic inflammation in the tissue surrounding the heel and over time this can lead to the accumulation of calcium deposits. Ankylosing spondylitis, for example, is one particular form of arthritis that frequently develops along with heel spurs. This condition can damage bones all over the body and even lead to the fusion of spinal vertebrae.

Symptoms
Although it may take years to become a problem, once it appears, it may cause considerable suffering. Because of proximity to the tendons, the spur is a source of continuous painful aching. The sensation has been described as "a toothache in the foot." When you place your weight on the heel, the pain can be sufficient to immobilize you.
Diagnosis
A heel spur is often seen on X-ray as a bony protrusion, which can vary in size. However, because a Heel Spur only indicates increased load on the plantar fascia, and not pain, an ultra sound may be required to assess other actual cause of the heel pain such and may include checking to see if the plantar fascia is inflamed or degenerated.
Non Surgical Treatment
The key for the proper treatment of heel spurs is determining what is causing the excessive stretching of the plantar fascia. When the cause is over-pronation (flat feet), an orthotic with rear foot posting and longitudinal arch support is an effective device to reduce the over-pronation, and allow the condition to heal. Other common treatments include stretching exercises, losing weight, wearing shoes that have a cushioned heel that absorbs shock, and elevating the heel with the use of a heel cradle, heel cup, or orthotic. Heel cradles and heel cups provide extra comfort and cushion to the heel, and reduce the amount of shock and shear forces experienced from everyday activities.
Surgical Treatment
Surgery involves releasing a part of the plantar fascia from its insertion in the heel bone, as well as removing the spur. Many times during the procedure, pinched nerves (neuromas), adding to the pain, are found and removed. Often, an inflamed sac of fluid call an accessory or adventitious bursa is found under the heel spur, and it is removed as well. Postoperative recovery is usually a slipper cast and minimal weight bearing for a period of 3-4 weeks. On some occasions, a removable short-leg walking boot is used or a below knee cast applied.
Prevention
There are heel spur prevention methods available in order to prevent the formation of a heel spur. First, proper footwear is imperative. Old shoes or those that do not fit properly fail to absorb pressure and provide the necessary support. Shoes should provide ample cushioning through the heel and the ball of the foot, while also supporting the arch. Wearing an orthotic shoe insert is one of the best ways to stretch the plantar fascia and prevent conditions such as heel spurs. Stretching the foot and calf is also helpful in preventing damage. Athletes in particular should make sure to stretch prior to any physical activity. Stretching helps prevent heel spurs by making tissue stronger as well as more flexible. In addition, easing into a new or increasingly difficult routine should be done to help avoid strain on the heel and surrounding tissue.
Will A Posterior Calcaneal Spur Cause Pain?
Overview
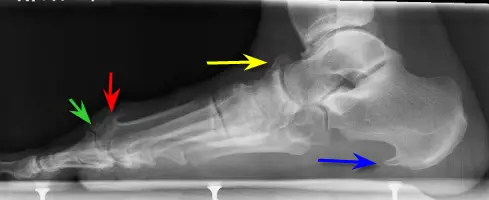
A heel spur occurs when calcium deposits build up on the underside of the heel bone, a process that usually occurs over a period of many months. Heel spurs are often caused by strains on foot muscles and ligaments, stretching of the plantar fascia, and repeated tearing of the membrane that covers the heel bone. Heel spurs are especially common among athletes whose activities include large amounts of running and jumping. Heel spurs often cause no symptoms but can be associated with intermittent pain, especially while walking, jogging, or running. Sharp pain in the heel can also be experienced when standing after sitting for a long period of time. Heel spurs can be a result of plantar fasciitis.
Causes
A heel spur is caused by chronic plantar fasciitis. Your plantar fascia is a thick fibrous band of connective tissue originating on the bottom surface of the calcaneus (heel bone) and extending along the sole of the foot towards the toes.Your plantar fascia acts as a passive limitation to the over flattening of you arch. When your plantar fascia develops micro tears or becomes inflamed it is known as plantar fasciitis. When plantar fasciitis healing is delayed or injury persists, your body repairs the weak and injured soft tissue with bone. Usually your injured fascia will be healed via fibroblastic activity. They'll operate for at least six weeks. If your injury persists beyond this time, osteoblasts are recruited to the area. Osteoblasts form bone and the end result is bone (or calcification) within the plantar fascia or at the calcaneal insertion. These bone formations are known as heel spurs. This scenario is most common in the traction type injury. The additional bone growth is known as a heel spur or calcaneal spur.
Symptoms
Some symptoms at the beginning of this condition include pain and swelling, and discomfort when pushing off with the toes during walking. This movement of the foot stretches the fascia that is already irritated and inflamed. If this condition is not treated, pain will be noticed in the heel when a heel spur develops in response to the stress. This is a common condition among athletes and others who run and jump a significant amount.
Diagnosis
A thorough history and physical exam is always necessary for the proper diagnosis of heel spurs and other foot conditions. X rays of the heel area are helpful, as excess bone production will be visible.
Non Surgical Treatment
In case of heel spurs rest is most important. Active sports, running, long walks etc should be avoided to start with. If you?re in a job that requires a lot of standing, take a few days off work. Rest (or reduced activity) is essential to allow the inflammation from becoming aggrevated. Furthermore, you can use ice packs (placed on the heel for 5-10 minutes) to ?cool down? the inflamed area. You may take anti-inflammatory medication or apply a topical inflammatory (i.e. a cream) to help reduce inflammation. In addition, there are some simple exercises that should be done daily to help relieve heel spur pain.
Surgical Treatment
More than 90 percent of people get better with nonsurgical treatments. If conservative treatment fails to treat symptoms of heel spurs after a period of 9 to 12 months, surgery may be necessary to relieve pain and restore mobility. Surgical techniques include release of the plantar fascia, removal of a spur. Pre-surgical tests or exams are required to identify optimal candidates, and it's important to observe post-surgical recommendations concerning rest, ice, compression, elevation of the foot, and when to place weight on the operated foot. In some cases, it may be necessary for patients to use bandages, splints, casts, surgical shoes, crutches, or canes after surgery. Possible complications of heel surgery include nerve pain, recurrent heel pain, permanent numbness of the area, infection, and scarring. In addition, with plantar fascia release, there is risk of instability, foot cramps, stress fracture, and tendinitis.